Is there any way to know whether someone has had Covid-19 in the past?
Dr William Hillmann: At this point, we don’t have a test to tell that. We are developing antibody tests to check for a prior infection, but those aren’t ready for clinical use yet. The only definitive way to know that you’ve had it is to get tested while you have it and to have that test be positive.
Could I have had it and been asymptomatic?
Hillmann: Coronavirus is actually quite a significant spectrum of symptoms, from people who are entirely asymptomatic and would have no idea that they have it to people with very mild, cold-like symptoms — runny nose, congestion, sore throat — to people with more flu-like symptoms — high fever, muscle aches, shortness of breath and cough. All the way up to people with severe illness, who we’re seeing in the hospital with respiratory failure, requiring ICU care. (Editor’s note: recent reports suggest that loss of smell and taste are also signs of Covid-19 infection.)
What percentage of carriers are asymptomatic?
Dr David Buchholz: Right now in New York, we’re only testing the sickest possible people. So we have no idea. However, there was a study in Iceland, which tested [a large segment of its] population, and 50% of the people who tested positive had no symptoms.
Are people who are asymptomatic also contagious?
Hillmann: A significant proportion of people who are totally asymptomatic are contagious for some portion of time. We just don’t know [for how long] at this point, because we don’t have the kind of testing available to screen for asymptomatic infections.
When people are symptomatic, they’re contagious. A day or two before they become symptomatic, they’re likely contagious as well. A virus builds up and starts to shed, and then after symptoms resolve, people can still be contagious for a couple of days. We have some evidence of viral shed even a couple of weeks after symptoms are resolved. It’s hard to know if that’s actual live virus, which is still able to infect somebody, or if that’s just dead virus that the body is shedding.
Should someone behave differently if they think, but don’t know for certain, that they have already had it?
Buchholz: We all have to be role models. If we’re all in it together, we all should be doing social distancing.
Hillmann: Since there’s no real way to know at this point who might have had it, unless you’re symptomatic, you get a swab and are definitively diagnosed with it, I would just act as if you hadn’t had it. Keep doing all of those things that we all should be doing at this point: social distancing and hand hygiene.
If I think I may have had it, do I have an ethical obligation to tell people I came in contact with? Even if it may in fact just have been a cold?
Buchholz: I would, absolutely. I’m in New York, and it was definitely in the community before we knew it. So, yeah, any family members and close friends, maybe somebody you work next to, I think I would just alert them, especially if it was in the last 14 days. If it’s been more than 14 days, they would have gotten sick by now if they had significant exposure.
Hillmann: It’s up to every individual about what they feel is right. If somebody is diagnosed with a case of coronavirus, I might feel a little bit more strongly that they should tell people because if you’re in close contact with a healthcare worker, it could have implications for precautions that healthcare worker needs to take.
If I’ve had it, can I get it again?
Buchholz: There’s not been any evidence that anyone’s gotten it more than once. Someone with a normal immune system that can react to the virus and get better should have immunity for quite some time, at least a year, if not lifelong.
There have been reports out of China suggesting people are testing positive for Covid-19 a second time. Most scientists think it is an issue around the inaccuracy of the testing and not that people are having two separate cases of the disease. — The Guardian
Experts
*Dr David Buchholz, senior founding medical director, primary care, assistant professor of paediatrics, Columbia University Irving medical centre
*lDr William Hillmann, associate inpatient physician director at Massachusetts general hospital
Why do some young people die of coronavirus?
Coronavirus hits the old hardest, but young people are dying too. Scientists say it may be down to genes or ‘viral load’, writes Robin McKie
It remains one of the biggest puzzles of the Covid-19 pandemic. The disease generally causes serious problems only in older people or those with underlying health problems. But occasionally it strikes down young, apparently fit individuals, including medical staff exposed to patients with the virus.
In some cases, previously undiagnosed conditions are later revealed but in others no such explanations are available, leaving scientists struggling to find reasons for the behaviour of the coronavirus.
Several theories have been proposed. Some researchers believe the amount of virus that infects an individual may have crucial outcomes. Get a huge dose and your outcome may be worse. Others argue that genetic susceptibility may be involved: in other words, that there are individuals whose genetic makeup leaves them more vulnerable to the virus as it spreads through their bodies.
This latter idea is favoured by virologist Michael Skinner at Imperial College London. “It is very possible that some of us could have a particular genetic makeup that makes it more likely that we will respond badly to an infection with this coronavirus,” he said.
An example of such susceptibility is provided by the herpes simplex virus, which causes cold sores. In some people, a mutation that affects cell receptors known as TLR3, in their central nervous system, leaves them unable to deal with the worst impact of the virus: they contract a disease called herpes simplex encephalitis, which can lead to seizures and convulsions in children.
“It could be that we are seeing a similar sort of susceptibility in some individuals who get Covid-19, and that leads them to suffer more acutely from serious side-effects,” added Skinner.
Others, however, suggest that the amount of virus that a person is infected with could be a crucial factor in determining their outcome. Such individuals are said to be affected by a high viral load.
“A person with a high viral load has more virus particles than one with a low load,” said virologist Alison Sinclair at Sussex University. “We do not yet know what impact viral load has on the symptoms of a person infected with Covid-19. Whether there is a link between a high viral load and worse outcomes is going to be important to find out.” — The Guardian
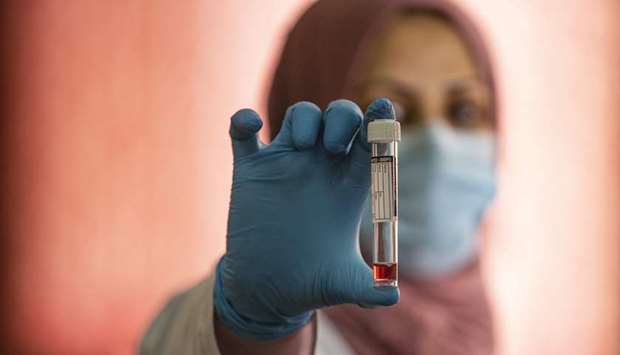
VTM: A member of the Covid-19 Crisis Cell holds a vial containing Virus Transport Medium (VTM), a substance that preserves nasal swab specimens while being transported to labs, produced at Basra university in southern Iraq. AFP
