By Ryder Diaz
A jiggly material called hydrogel, similar in texture to Jell-O, may help mend damaged cartilage, keeping joints moving and people active.
The slippery hydrogel can jump-start cartilage growth and reduce pain, compared with the most common procedure now used in surgery, a group of scientists reported in the journal Science Translational Medicine.
Although the study tested the new approach on a small group of patients, hydrogel shows promise in becoming the standard for a simple, low-cost procedure, said Garry Gold, a Stanford University professor and an author of the study.
Cartilage acts as a cushion between bones, allowing them to glide smoothly past each other during activities like climbing a flight of stairs. An injury can create a pothole in the cartilage, Gold said.
Without the padding, bones painfully scrape against each other. That can limit exercise and can lead to more serious surgeries. About 750,000 people get artificial knee replacements in the United States every year due to injury or disease in knee cartilage, according to the American Academy of Orthopaedic Surgeons.
“I know what the impact of having an injury like this can be on your life and on doing the things you want to do,” Gold said.
Gold, a former marathon runner, was stopped in his tracks by damage to cartilage in his knee. But for him, research into improving cartilage repair is more than personal.
“It’s not going to help me; I’m not going to be running again,” Gold said. “But it may help some of my students or some of the athletes I work with here at Stanford.”
Damaged cartilage is hard to fix, especially in older people who don’t heal as well. “It doesn’t repair itself,” said Jennifer Elisseeff, a professor at Johns Hopkins University and a co-author of the study.
Unlike other parts of the body, cartilage does not receive a supply of blood, which carries the nutrients needed for healing.
“There are not many great therapies out there for cartilage,” Elisseeff said.
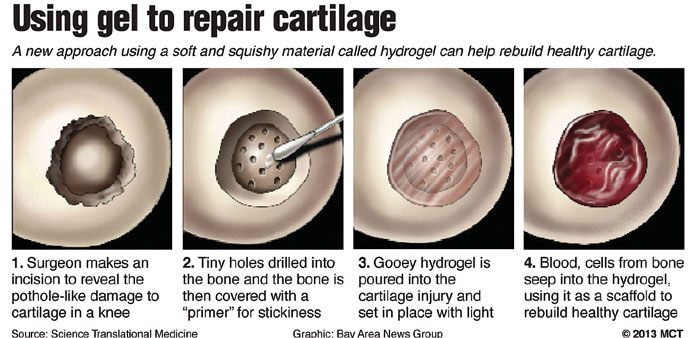
One common method, called microfracture, drills tiny holes into the bone in the spot where the cartilage is missing. Blood and stem cells from the bone marrow spill into the damaged area. Surgeons hope these cells will grow into new, healthy cartilage.
But because there is nothing for the cells to hold onto, they often grow in a sloppy way, creating scar tissue. “The scar cartilage, it’s less durable,” Elisseeff said.
That poor-quality cartilage can break down and disappear in two years, Gold said. Patients can experience the return of pain and the arrival of arthritis as more healthy cartilage disappears.
The new procedure tested by Gold, Elisseeff and colleagues added hydrogel to the microfracture technique.
Here, exposed bone is coated with a primer before holes are drilled. Then the gooey liquid hydrogel is poured in to fill in the missing cartilage, sticking to the primer. Light is used to set the gel, similar to the way a dentist uses light to solidify a filling in the cavity of a tooth.
The hydrogel creates a scaffold for the blood and stem cells from the bone marrow to cling to as they grow into healthy, new cartilage, Gold said. As new cartilage grows, the hydrogel dissolves.
After six months, the team found that patients treated with hydrogel had less pain and more healthy cartilage filled the pothole than the traditional approach.
“This is what we think of as the future of joint replacement,” said Kevin Stone, a surgeon and researcher with the Stone Clinic in San Francisco, who was not involved in the study. Instead of replacing damaged joints with metal or plastic, Stone said that using materials such as hydrogel can rebuild better cartilage, naturally.
“We’re encouraged but still a little bit away from having a routine surgical procedure,” Gold said.
For the technique to be in the hands of surgeons, it would need to be tested on a larger group of patients for a longer period of time and approved by the Food and Drug Administration.
The technology has been sold to BioMet, a company that designs medical therapies, according to Elisseeff.
“The best we could hope for is that it doesn’t break down quickly, relieves pain and slows the progression of arthritis,” Gold said.
Because options for cartilage repair are few, almost a decade ago Gold enrolled himself in an experimental cartilage study. Even though that procedure — which did not include hydrogel — did not improve his knee problem, he wanted to help move research forward. Also, he didn’t have much to lose.
“If you’re in an area like cartilage repair, where existing treatments work but not that well, it might be good taking a chance,” said Gold. — San Jose Mercury News/MCT